Beyond AMR: microbial adaptation and disinfection strategy
Author: Arxada Professional Hygiene Team

Efficacy as the ultimate benchmark
For both the manufacturer of a disinfectant and the facility implementing it, the primary objective is appropriate efficacy. In high-stake environments like healthcare, a lack of biocidal performance is not a minor oversight; it can lead to critical failure. Inadequate disinfection as part of infection control can result in Healthcare-Associated Infections (HAIs), increased mortality rates, or the survival of pathogens leading to wider spread of infection.
However, achieving the necessary efficacy can be challenging. A product - whether a surface disinfection spray, pour - on products, surface disinfection wipes or dilutable concentrates for large surface disinfection - is only as effective as the precision with which it is applied.
The integrity of the method: Why producer instructions are critical
In the professional hygiene sector, a disinfectant is a validated tool, not merely a chemical solution. Its efficacy is a result of a strict relationship between the formulation and its application protocol. When a manufacturer specifies a way of use, they define the exact parameters (i.e. - concentration, contact time, and application method) required to define the intended disinfection level, ranging from Low-Level to High-Level Disinfection (HLD). All these performance claims are strictly supported by the mandatory EN standards we have discussed in our previous technical deep-dive; you can review that full article on efficacy benchmarks here: Raising the bar: understanding the new standards for disinfectant efficacy in medical settings
To ensure proper infection prevention and control, the disinfectant must be selected based on the clinical risk profile:
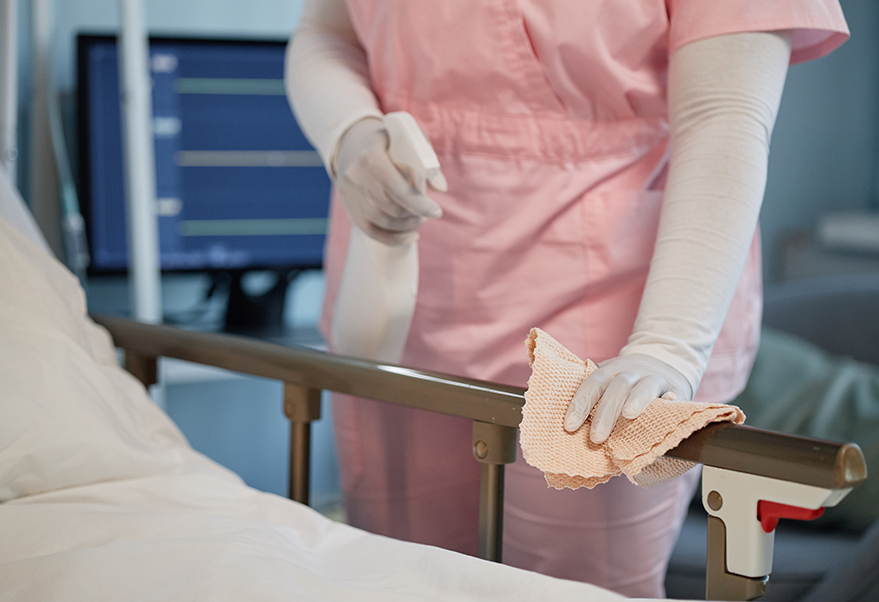
Low-Level Disinfection (LLD): For non-critical surfaces (e.g., bed rails, floors) to eliminate vegetative bacteria, yeasts and enveloped viruses.
Mid-Level Disinfection (MLD): Required for resilient pathogens like Mycobacterium tuberculosis or non-enveloped viruses.
High-Level Disinfection (HLD): Mandatory for high-risk areas and devices (e.g., endoscopes). HLD should be designed to target microorganisms, including high concentrations of bacterial spores.
Even if the correct agent is selected, with full consideration of its material compatibility and efficacy level, the process can still fail. What else can go wrong? The answer lies in the correct way of use.
The biological cost of non-compliance: Understanding microbial adaptation
The Karpiński Adaptation Index (KAI)[i] – Quantifying the failure of disinfection
Microorganisms like bacteria and fungi possess a remarkable ability to survive when the Instructions for Use (IFU) are not strictly followed. This is the path to microbial adaptation.
Sub-lethal stress: When a disinfectant is applied at concentrations lower than required (e.g., 20% to 45% of the intended dose), it does not kill the population; it stresses it.
The adaptation curve: during microbial growth, bacteria change morphologically to survive. Professor Karpiński’s research highlights an alarming trend: while many microbes are killed at mid-range concentrations, substances like sodium hypochlorite allow for adaptation up to 100% of the commercial concentration.
Defining the threshold: adaptation risk
Microbial adaptation risk
The effectiveness of any disinfection protocol is contingent upon maintaining the integrity of the active substance's concentration and contact time. When these parameters are compromised, we may face the risk of microbial adaptation - a process where bacteria and fungi adjust to surviving in the presence of sub-lethal doses of an active agent. The Karpiński Adaptation Index (KAI) provides a standardized metric to evaluate this risk by comparing the concentration at which adaptation occurs to the standard commercial dose.
Low-risk chemistries (Low KAI): Substances like Polyhexamethylene biguanide (PHMB), Boric acid, or Povidone-iodine. Adaptation occurs at levels 20 to 100 times lower than the commercial dose.
High-risk chemistries (High KAI): Substances like sodium hypochlorite (KAI ≥ 1.0) show a high risk because adaptation can reach the full commercial concentration, leading to a total loss of efficacy.
Preventing unintended dilution in clinical settings
Selecting the right chemistry is only half of the battle. To prevent microbial adaptation and ensure patient or consumer/customer safety, the focus must remain on the precision of the application.
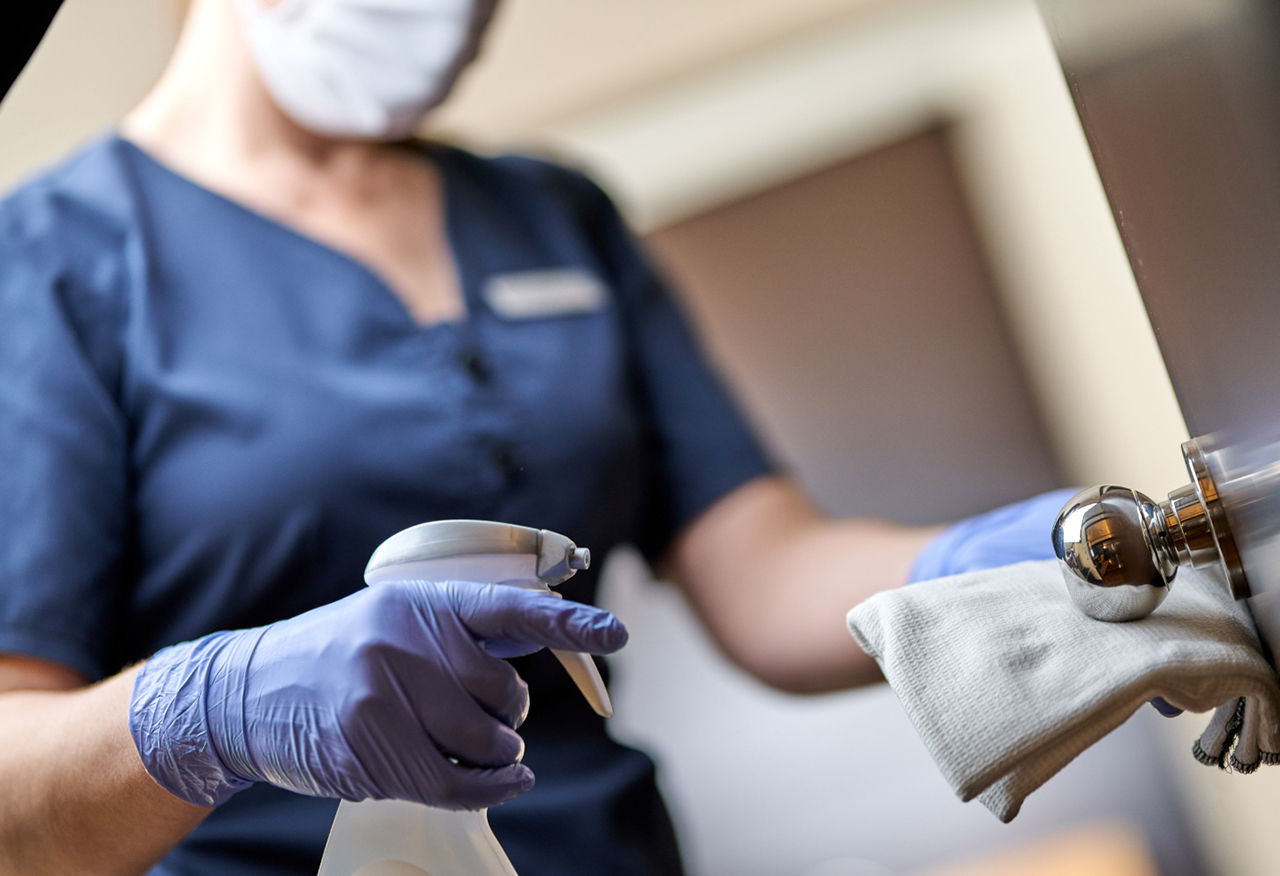
Prevent unintended dilution: Compliance with the Method of Use extends beyond the mixing bucket.
A common 'critical gap' in infection prevention occurs when a disinfectant- whether a Ready to Use (RTU) product or a solution prepared from concentrate - is applied to a surface still wet from prior cleaning, or when concentrates are not precisely diluted. Both scenarios lead to unintended dilution, resulting in sub-lethal concentrations that allow microorganisms to survive and in special cases, to adopt.
To ensure expected efficacy, surfaces should be allowed to dry before disinfectant application or be properly managed to ensure the disinfectant reaches the pathogen at its full intended strength.
Strict adherence to the manufacturer-specified contact time is essential to ensure full biocidal efficacy.
Whether using Ready to Use (RTU) surface disinfection wipes or solutions prepared on-site from concentrates, strict adherence to manufacturer-instruction of use, like required contact time or dilution ratio, is non-negotiable. For facilities using concentrated systems, implementing automated dosing or rigorous staff training on preparation ensures that sub-lethal dosing is avoided.
Conclusion
We secure the future of infection prevention and control by moving away from substances with a proven high risk of microbial adaptation. For this chemistry, the KAI (Karpinski Adaptation Index) is 1.0 or higher, meaning bacteria can survive even at full commercial concentrations.
It is critical to minimize the likelihood of human error on the final concentration and contact time during use; this can support the prevention of developing of persistent microorganisms and reservoirs within biofilms. By prioritizing solutions with multi-target mechanisms of action, we significantly hinder the microbial adaptation process and effectively break the chain of transmission for multi-drug resistant organisms (MDROs).
[i] Karpiński, T. M., Korbecka-Paczkowska, M., Stasiewicz, M., Mrozikiewicz, A. E., Włodkowic, D., & Cielecka-Piontek, J. (2025). Activity of Antiseptics Against Pseudomonas aeruginosa and Its Adaptation Potential. Antibiotics, 14(1), 30.
Get in touch
For more information or to stay up-to-date with our news, please contact us or sign up to our e-Newsletter.